Introduction
Percutaneous laser disc decompression (PLDD) is one of the so-called “minimally invasive” treatment modalities for contained lumbar disc herniation. The treatment is performed percutaneously, so morbidity is expected to be lower and convalescence period is postulated to be shorter than for conventional surgery. Because of the minimally invasive nature and the fact that return to work is usually possible within a few days after treatment, PLDD appears to be an interesting alternative to conventional surgery; however, considerable skepticism still greets PLDD.
Review
Sixteen clinical trials were included in this review, representing a total of 1579 patients. Trials were only included if they provided enough information on techniques used in the procedure (laser type, parameters used, etc) and no additional techniques such as endoscopy were used. Clinical trials were only included when they addressed the outcome of PLDD.
Method
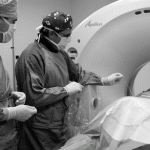
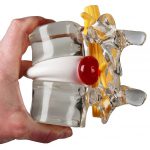
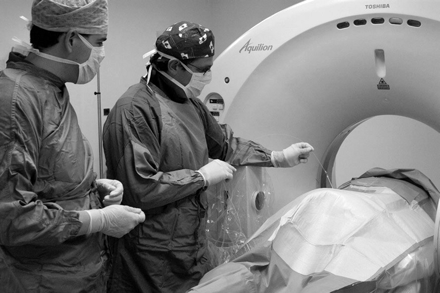
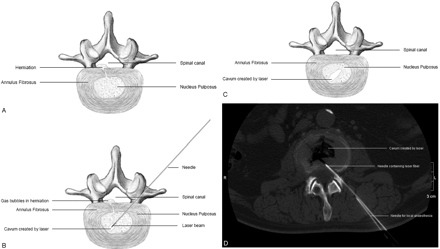
The procedure is conducted under local anesthesia of the skin and underlying muscles. After assessment of the correct disc level by using fluoroscopy, a hollow needle is inserted 10 cm from the midline, pointing toward the center of the disc. When the needle is in place, its correct position is verified by using biplanar fluoroscopy, sometimes in combination with CT imaging. A laser fiber (0.4 mm) is inserted through the needle into the center of the nucleus pulposus. Laser energy is then delivered into the nucleus pulposus to vaporize its content and reduce intradiscal pressure
Result
Success rates in the larger studies varied from 75% (95% confidence interval [CI], 69%–81%) to 87% (95% CI, 80%–94%). The definition of “successful outcome” varied strongly between the different studies, depending on the outcome measures used. The duration of follow-up ranged from 3 to 84 months. Because of insufficient improvement of symptoms or recurrent herniation, 4.4% to 25% of patients received additional surgical treatment. In most cases, surgery revealed the presence of free fragments in the spinal canal.
Conclusion
The main determinants for heat penetration are water absorption, which varies with laser wavelength, and the duration of application of laser energy. For example, in case of a 980nm diode laser, the initial power setting is 4 W, whereas the average power in trials by using a 1024nm Neodymium-YAG laser is 17 W. Pulsed delivery of laser energy is used to allow dissipation of heat generated by a single pulse before administration of the next pulse, thereby avoiding excessive heating of surrounding tissues.
Refrence
Percutaneous Laser Disc Decompression: A Review of the Literature
Schenk, P.A. Brouwer, W.C. Peul and M.A. van Buchem
American Journal of Neuroradiology January 2006, 27 (1) 232-235;